The First Rule of Back Club Part II
A last meeting with the surgeon, Mr Tucker on Wed 3rd May, to review the last MRI results. One percent of me hopes there will be a last minute reprieve and surgery is not actually necessary and my spine will gradually straighten itself out over time. Obviously not forthcoming but the laconic Mr Tucker does at least proffer one olive branch - I don’t need to be at the hospital until 10am and not 8am as previously stated. Furthermore if I get up early enough I am allowed a small breakfast. Anything to avoid the dreaded nil-by-mouth
On the day
The morning of the 5th is lovely, both meteorologically and literally. We go for a brief, and admirably early family walk with Van our border terrier. Then Van gets dropped off at my parents (still in bed) and Scout gets dropped off at school. I am reasonably sure we got that the right way round. It is all a beautiful distraction on a clear late spring day from the impending trauma of major spine surgery. And that in itself, I am sure is worth so much in terms of approaching the day in a calm, positive and happy state of mind.
Bantam weight
Then Donna and I get on a train to Marylebone and a brief cab ride to the hospital. A few more blood tests and then I am weighed – 71.5kg! Exactly the same as my last surgery in 2013 and the exact number I have been aiming at since Xmas. This weight loss is all due to the 5:2 diet and the limited gentle exercise programme I have been following from Alex (osteopath) and Fiona (physio).
Speaking of Alex
Speaking of Alex – he pops his head around the door and will be in surgery as an observer. He has been with me through this injury, and its day to day management since day one, and has been a steady hand and friend.
Then a brief visit by Mr Tucker and the anaesthetist, telling me in excruciating detail what they are going to do this very afternoon and how I am going to feel, but in a very reassuring manner. Oxymoron.
Walking
And then I walk into from my room to theatre. Strange as it sounds even this is reassuring in its normality. It just seems to be Mr Tucker’s way of smoothing the whole process of giving yourself up to becoming a virtually helpless patient. And in combination with my relaxing morning with my family and chat with Alex I walk into theatre very calm, smiling with absolutely no apprehension. Truly. Go back to my point five from my last Journal’s My Back Surgery Top-Tips point number five –
“……..and if you just have to have surgery then try to mentally prepare by being as positive as possible about that fact and event”
Missed Afternoon
And some seven hours later I wake up in ICU looking up at my wife in a tramadol fug (me not her). This is my third operation in four years. This is not my first rodeo. I know the rules:
1. Accept the weirdness
2. Punch the morphine when you hear the beep
3. Take in information in manageable bite-size chunks
4. Trust your doctors
Donna (not her first rodeo either) persistently repeats, two things she knows that I need to know. Number one that Mr Tucker, in cutting away more of my rib, managed to the access the front of my spine, without collapsing my lung again so I don’t need a chest drain. And two, he has managed to straighten my spine back to zero degrees from its previously kyphosed distortion. Both these snippets from the cutting-room floor are gratefully received.
Only when I laugh
The whole ITU experience is like a Timothy Leary house party. I don’t remember much and yet I remember every single minute, tranquillised but not anaesthetised. I vaguely remember my friend Justin, who is an ITU consultant at a different hospital, smoothly move around the room like he is on castors, quietly taking everything in. He says a few plain words of reassurance and then he is gone. It is incredibly reassuring that he came at all. I don’t think anyone else noticed he was even here. Maybe he wasn’t.
Hard drugs and soaked in adrenalin
Sometime over the weekend I am moved back to the ward. I really don’t remember this. And you know what I feel tremendous. Mr Tucker (who sees me on Saturday and Sunday) cautions me about undue optimism. He gently explains that after major surgery the body comes out soaked in adrenalin and hard drugs, that a feeling of euphoria and general immortality is not uncommon. But once the worst soporific effects of the general anaesthetic have worn off there can be a physical and mental cliff.
I don't like Mondays
And Monday sees the plunge into deep pain, nausea, claustrophobia and depression. I have never felt so utterly depleted and defeated. The hangover of powerful drugs and long surgery. It was always going to happen but I don’t remember it being this bad last time. The whole working week is pretty much spent in this trough. Mr Tucker comes to see me every day without fail. This is vitally important to a patient and should be added to my top tips for surgery - make sure the surgeon will see you every day post-surgery. Not one of their team but the actual consultant. Mr Tucker even made the effort to come and see me on Saturday and Sunday. Hugely impressive; last time I never saw the surgeon again for months, by which time I was already struggling. The surgeon's constant contact with the patient is absolutely essential, both clinically and in terms of the confidence and therefore recovery of the patient.
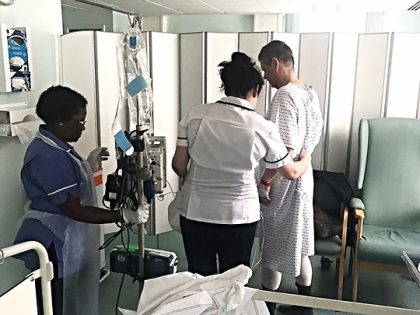
Walking like Windy Miller
My first steps with the physio were actually pretty early – I can’t remember exactly when. But I do remember the feeling of being off balance and flat-footed. I rationally know this is because my sagittal balance has changed and with it my centre of gravity. But as I clump around the bed like Windy Miller there is bugger all I can do about it. So Windy Miller it is. The attitude to spine surgery has changed over the years and the orthodoxy now is to get patients up and walking as expeditiously as possible. The new protocol is that loaded bone is good bone, so get up and get moving. Even if you don't feel like it and forget that you have a processional train carrying your respective drains and tubes.
Gate happy. Taxi!
At the first mention that I may have ticked all the discharge criteria, I ask Donna to call a cab. It is true that I still have a lot of pain, feel nauseous, and generally very weak. But Mr Tucker persuades us that these symptoms will pass more easily in the home environment. Once again this is the difference between having your surgeon on the ground with you to make these finessed clinical calls. He was absolutely right and a couple of days at home and the nausea has passed and I am feeling generally brighter. Next step is to gradually 'mobilise' which largely means trying to walk less like a puppet and more like a proper human. No strings attached.